Have you had a fracture?
This article explains how Phillip Wilson can significantly speed up your post fracture healing.
Case studies:
Recently a 14 year old girl attended with a 2 year history of pain post fracture in her knee. Her sport had been almost nil in those important years and was still suffering with pain and swelling.
The second patient included was a 7 year old boy who had suffered an ankle fracture whilst skiing. Post fracture he was struggling to walk properly couldn’t run and was suffering pain in his knee.
A third was a patient who runs and competes in hurdles presented with pain in his back, thorough assessment didn’t present as a typical back pain and further review located a fractured big toe from 2 years previously causing his problems.
See below
Fractures:
Humans are made up of skin, soft tissues, bones, tendons, ligaments, and muscles, which work together to enable the gross and fine motor function required to carry out daily tasks from writing, dressing, and washing, as well as highly skilled tasks such as operating machinery and playing musical instruments to walking, running and lifting. It is this highly precise function that means even minor injuries can risk causing significant handicap.
Post-fracture stiffness and loss of range of motion (ROM) in the adjacent joint are a common complication of fracture. Stiffness, or more accurately, a limitation in the ROM, is a potential complication after any intra-articular or extra-articular injury.
Following a fracture damaged structures will repair through a cascade of processes, aiming to restore the original tissue integrity. All of the causes of a traumatic injury can lead to stiffness through scarring, contractures, and damage to articular surfaces, which lead to disruption of the normal anatomy. Pain and swelling following injury are common, leading to immobility of the joint followed by longer-term stiffness.
Post-traumatic joint stiffness can be further influenced by the development of chronic regional pain syndrome (CRPS). CRPS is due to an abnormal inflammatory response following trauma due to sustained sympathetic activity. This can lead to stiffness, as well as pain, swelling, vasomotor disturbance, and trophic skin changes.
Rarely, hypertrophic ossification following trauma can be post fracture following trauma; this leads to the formation of atypical bone in tissues, contributing to stiffness.
When soft tissues are damaged due to trauma, subsequent wound healing has 3 phases; inflammatory, proliferation, and maturation. Firstly, the inflammatory phase is triggered by the disruption to the vasculature leading to exposure of the subintimal layer, with the movement of inflammatory leukocytes to the site of injury. Resultant oedema leads to disruption of the gliding movement of the joints. In the long term, this protein-rich exudate will become scar tissue resulting in adhesions forming, causing further disruption to normal movement. During the proliferative phase, there is a deposition of type III collagen within the joint capsule, ligaments, and tendons. In the final phase, there is scar maturation and contracture; this results in disruption of a joints’ normal anatomy and subsequent joint stiffness.
Clinical signs of inflammation can be seen on examination, such as oedema, erythema, pain, and reduced range of movement. Differences between active and passive movements can help to differentiate between a joint versus a musculotendinous cause of the joint stiffness. If active and passive motion is the same, it’s more likely to be the joint itself restricting movement; if the passive movement is greater than the active movement, movement is likely to be restricted due to a musculotendinous reason.
Case study 1:
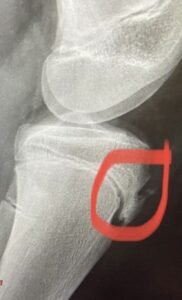
A 14 year old girl, previously very active had fallen off her bike directly onto her knee 2 years previously. Her Xray had described a patella insertion irregularity. She suffered swelling around her tibial tuberosity (the point you kneel on at the top of the tibia) this is where the patella tendon inserts onto the the tibia. (see X-ray above)
She had attended NHS physio and was given exercises which hadn’t helped and even made it worse. She then saw an orthopaedic surgeon who advised it was Osgood Schlatters which is growing pains and there is inflammation on the tibial tuberosity. However on examination this did not present as growing pains, rather a post traumatic irritation/ small fracture to the tibial tuberosity, this had then led to chronic inflammation and Chronic Regional Pain.
I treated this with specific soft tissue massage and frictions which stimulates the tissue to break the pattern of chronic inflammation and pain. We soon progressed on to stretches and strengthening and 1 month later she was back to sport and an active life again.
Case Study 2:
A 7 year old boy had fractured his tibia whilst skiing. He was placed in a plaster with his foot slightly down, this may have been done to maintain the position of the fracture site. He had the plaster removed and had been discharged from the fracture clinic. His parents were worried as he was walking funny and couldn’t run.
His whole ankle joint had stiffened significantly and he couldn’t bend his foot up, as a consequence his knee was hyperextending (bending backwards) and his knee ligaments were being stretched. I was very happy they brought him along when they did or he would have had an irreparable knee as well as a stiff ankle.
I worked on high grade joint mobilisations of the ankle, this is achieved with a shearing motion using my power to stretch the joint to increase the range of motion which can’t be achieved just with exercises.
He responded very well and now has a normal functioning ankle and knee and has returned to sport.
Case study 3:
A young chap who performs at a high level in hurdles had been struggling with back pain. When I assessed his presentation didn’t seem like a normal back pain and when I performed my full biomechanical assessment I discovered his big toe hardly moved. I filmed him running on the treadmill in slow motion and this confirmed his odd gait. I worked solely on toe mobilisation and manipulation and after only a few weeks he was back to full range in the toe and his gait had returned to normal, his back pain cleared and he is now participating in all his sport.
Whatever your age or level of function post fracture stiffness can affect you and we will help you to quickly become free of pain and return to full range.
Phillip Wilson
Consultant Physiotherapist.
Call 01962 714979